The Wallics "Have Been There And Back"
Frank arranged a follow-up examination with his primary doctor. Frank complained that he was plagued with a shortness of breath when he exerted himself. His doctor ordered further x-rays. The films showed an accumulation of fluid on his left lung. A CT scan was ordered and Frank was referred to a pulmonary specialist.
Frank's condition grew worse. In mid-August, he had so much pain in the bottom of his left lung, chest and back that he nearly passed out from the constant coughing. Breathing became a struggle. Frank was anxious to get to the pulmonary doctor. He wanted to know what was happening inside his lungs.
After reviewing the CT scan and the x-rays, the pulmonary doctor arranged for Frank to be admitted to the hospital as an outpatient so that they could drain the fluid in his lung lining. On August 22, 1997, Frank's wife Sondra and their daughter-in-law stood in the hallway of the hospital and watched Dr. Jones [the doctor's name has been changed] draw 2000 milliliters of ugly fluid from Frank's left lung. The doctors sent the specimens to pathology for testing.
The Wallics met with Dr. Jones on August 28, 1997. He explained the results of the pathology tests. Frank had malignant mesothelioma. Dr. Jones had treated mesothelioma patients before. He advised Frank and Sondra that some of his patients have lived as long as ten (10) years with just having the fluid drained when the shortness of breath and pain increased. Others, he disclosed, died relatively quickly, within eight (8) to twelve (12) months after the initial diagnosis. It did not sound like the doctor was advising any aggressive treatment plan.
The Wallics searched for a second opinion. On September 4, 1997, they met with Dr. Cecile Rose at the National Jewish Hospital in Denver, Colorado. Dr. Rose is a renowned expert in asbestos-related diseases. During this consultation, Dr. Rose explained a new program that could determine if Frank would be a suitable candidate for the extrapleural pneumonectomy (EPP).
Dr. Rose advised that, statistically, the life expectancy of a MM patient from the date of diagnosis was eight (8) to twelve (12) months. She explained that the tumor usually attacks one lung and as the tumor gets larger it hardens, engulfs the lung and heart, and arrests the heart muscle. A temporary "fix" to stop the fluid from accumulating, she said, was to use talc or a glue-like substance that acts as a Band-Aid by keeping the cancer from oozing.
Dr. Rose also explained that another temporary measure was to insert a tube and have the fluid drained into the stomach or the bowel area.
The Wallics appreciated Dr. Rose's candor (I have taken her deposition before and agree with the Wallic's that Dr. Rose is very smart pulmonary doctor with excellent bedside manner). The Wallics needed a "time out" to carefully review their options.
On September 5, 1997, Dr. Jones removed about 2700 milliliters of fluid. After this painful procedure, Frank and Sondra needed more time. Frank, according to Sondra, was preparing to die. Their son, Tierney, gave them new hope. He worked with a woman whose father had the same surgery described by Dr. Rose -- the EPP. This patient was doing fine after over three (3) years. After a week of rest and recuperation, Frank's enthusiasm for the surgery was restored. The next step was to find a thoracic surgeon who could perform this complicated surgery.
They first looked in their own backyard and found Dr. James Mault. Dr. Mault had just relocated from the Duke University Medical Center to the University of Colorado Medical Center. They learned that Dr. Mault had been performing this delicate operation for four years.
On September 19, 1997, Frank had another 850 milliliters of fluid drained from his chest. Dr. Jones expressed his concern that Frank's tumor was getting larger and he urged Frank to aggressively pursue the surgery. Frank's primary care physician was in contact with Dr. Mault and was instrumental in setting up the referral. He helped arrange the pre-surgery testing that Dr. Mault would rely upon to determined if Frank was a suitable candidate for the EPP surgery. The tests were taken the week of September 22, 1997.
On September 29, 1997, Frank and Sondra met with Dr. Mault. Dr. Mault was very open and provided the Wallics with a wealth of information. He explained the surgery and stressed that he still needed to review all of the tests before a final decision to operate could be made. That following Wednesday, a doctor from the University asked Frank to come in for a "GI" test. They explained to Frank that this test was necessary to determine if the tumor had invaded the heart. If it had, then Frank would not be a candidate for surgery.
Frank was given drugs to help him relax and his throat was sprayed with a local anesthesia to deaden it. A tube was inserted inside his throat and pushed down into his stomach. This scope would take an ultrasound of his heart and search for signs of the cancer. There was no tumor and the pre-op work was scheduled for Monday, October 6, 1997.
About 9:00 a.m. Tuesday morning Frank was hooked up to several tubes and monitors for the eight (8) hour surgery. He was in intensive care for approximately two (2) days. Sondra recalls that when the family saw him for the first time in ICU he had a large needle protruding from his jugular vein where the chemotherapy drugs and pain medications were administered during the surgery. The doctors had left it in place as a precautionary measure if further surgery was needed. Seeing your loving husband with a needle in his neck is not easy, but Sondra was overjoyed to see Frank. She couldnt wait to give her husband a big hug.
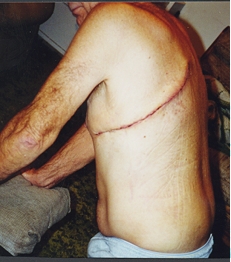
After the surgery, Frank's chest looked like a World War I battlefield. He had a one (1) inch incision that ran down like a trench from the 6th rib on his back around to the front under his left breast. He had a second incision (not visible, but under the skin) below his last rib where they reconstructed his diaphragm. This gave Frank the most pain. He was given percodan, which made him uncomfortable. Frank has been taking extra-strength Tylenol every four (4) hours.
When he first came home from the hospital, Frank could not lift his arms over his head. Sondra would help dress, feed and bathe him. Frank was very weak and had lost weight while the tumor was growing so rapidly. The Wallics were determined to refortify Frank's immune system and strength. They bought a juice extractor, which, upon reflection, they wished they had used well before the surgery. They began a program of 3 glasses of carrot juice daily - sometimes adding parsley, celery, beets a vitamin/mineral supplement. Also, 3 cans of Ensure Plus, which they alternated with Ensure /high protein per day. The Wallics have strongly endorsed the following three books, which have helped them build a solid diet program: "What to Eat If You Have Cancer" by Maureen Keane, "The Juiceman's Power of Juicing" by Jay Kordich, and "Juicing for Life" by Cherie Calbom.
Frank was more comfortable sleeping in the recliner than in the bed. He slept best between 8:00 p.m. and midnight. He then woke up and stayed awake till 5:00 a.m. He took naps during the day. Finally, about 3 weeks after surgery, Frank was comfortable in bed and his sleep pattern gradually became more stable, although a full nights sleep was still rare.
Frank and Sondra assumed that his mesothelioma was in Stage 1, but after visiting with Dr. Mault three (3) weeks after his release from the hospital, they learned that Frank was actually in Stage 3. The raging cancer had spread to his lymph nodes and the concern was that it had spread to his major organs. An ultrasound provided some good news: the tumor had not spread to his liver.
Now, it has been 7 weeks since the surgery and the Wallics have resumed their daily walks around the yard. At first, Frank was a little light headed but now he can shower, ride his exercise bike and drive the car. One morning he even fixed the water hose on his jeep. We all know a lot of otherwise healthy 68 year old husbands who fake an injury to avoid working on the family car!
Frank has actually gained 3 pounds ( he now weighs 152 lbs) and feels a little stronger. The radiation and chemotherapy will begin in a couple weeks (Dec. 5th). The regime is supposed to be a mild one. They will see.
Frank's daughter and her husband drove from Idaho to Colorado to be with the family to give love and support before, during and after the surgery. According to Frank she was a tremendous help.
For Frank and Sondra, nothing can exceed the joy and excitement when they will be able to return to normalcy.
The Wallics are dear people who want to extend a friendly hand to others similarly situated. "Our hearts go out to all those families that have just been told they have `malignant mesothelioma.' We want them to know we understand the horrible stress, sleepless nights, anxiety and anxiety attacks because `we've been there.'"
The Wallics want to help. They have volunteered their email address, which is sfwalli@juno.com
The Wallics contacted me so that we could tell others about their experience and also to advise patients in the midwest about Dr. James Mault. I spoke to Dr. Mault on the phone and was impressed with his interest and enthusiasm in helping mesothelioma patients. I learned from Dr. Mault that he is preparing to establish at the University of Colorado a phase II protocol using onconase. I was impressed with his knowledge of all the recent "cutting edge" developments for treating mesothelioma.
Based on the Wallic's positive endorsement, we notified the family of a 50 year old Nebraska man that Dr. Mault was available. Dr. Mault scheduled him for surgery within ten days of their first contact. Please see the letter from Lisa Whiting .
** POSTED DECEMBER 4, 1997 **
Frank Wallic passed away on February 6, 1998


