 Memorial Sloan Kettering New York, NY 9/15/99
Memorial Sloan Kettering New York, NY 9/15/99
Introduction to the "M" word
In July 1999, my husband,
Allan Ostling, was hospitalized with shortness of breath and a partially collapsed right
lung due to being filled with fluid. A pulmonary function specialist was
called in and during the initial questions from the doctor, I listened
to a lot of fairly routine questions regarding previous medical and work
history. But the doctor kept returning to questions regarding exposure
to asbestos. I knew the answer myself to that particular question. For
years, Allan has mentioned the huge amounts of asbestos he had encountered
during his career at Inland Steel. One of his comments to myself and our
friends was, "We would wade knee-deep in asbestos."
During the conversation, the doctor mentioned several medical problems
associated with fluid in the lung, stating he would methodically pursue
the cause. One of the things he mentioned was a word that I had never
heard of before. I remember it was a long word and began with an "M".
After leaving the hospital that evening, I went home to my computer, got
on the Internet and typed in the word "lung". To my sorrow,
there was more information than I could handle in my present emotional
state. I was worried sick about Allan and felt sure this was no little
problem we were dealing with.
The next day, when the doctor came in, he had more questions. Again the
topic of asbestos was approached and once again, I heard the "M"
word. That evening found me back on the Internet and much to my horror,
I found the "M" word - MESOTHELIOMA.
The Search for Answers
When I read the symptoms, read how someone contracts this dread disease,
read how someone is exposed to it and read the time frame involved…….
I knew. I started printing everything I could find on the subject from
a variety of web sites. Every one was more depressing than the last. But
they all had one thing in common……there is no cure.
I kept all this information in the back of my mind hoping not to have to
tell Allan what we might be facing. But, every night, I was back on the
Internet trying to find out more. I had alerted several family members
to the possibilities so if the time came, they would have some inkling
of what he might be facing.
All of Allan's tests during that hospitalization were inconclusive.
We were then referred to a thoracic surgeon to go in and get tissue samples
for possible identification. During the first appointment, we listened
to more questions regarding asbestos exposure and then this doctor also
said the "M" word. I think that was the first time Allan actually
heard the word and asked for an explanation. The surgeon explained, while
cautioning us not to jump to conclusions. There were other possibilities
to consider. Surgery was scheduled for the end of that week.
The Grim Diagnosis
On Friday, August 6, 1999, Allan underwent a right thoracotomy with multiple
biopsies of the pleura. The surgery did not begin until 8:30 PM and it
was midnight before the doctor came out to the waiting room. I could tell
from his walk and the look on his face. He sat down next to me and tried
to explain the procedure he had just completed, indicating that he tried
to scrape some of the tumor to allow for some stalling of the lung re-filling
with fluid. He said he had taken multiple wedges for pathology and for
final clarification; these would be sent to Mayo Clinic for confirmation.
During the surgery, they had done the preliminary frozen section, and
it was his and the pathologist's opinion that we were dealing with
a diagnosis of mesothelioma. I asked him about any further surgery, and
he indicated it was not possible. I asked about removal of the lung, and
he said it was not done in this case. I asked him if it was possible to
stage it, and he said we do not stage at this point. When I pressured
him for a guess, he indicated most probably a Stage IV. His final comment
was, "I'm very sorry."
I spent the next day, Saturday, in intensive care with Allan. His spirits
were good. He asked the question, and I evaded it. I did tell him the
pathology would be sent to Mayo's. When the doctor came in, I asked
him if he was going to tell Allan what he found, or should I. He stated
he wanted him to rest for this day, and would tell him in the morning.
He broke the news to Allan on Sunday, but still said we had to wait for
final confirmation from Mayo's. After 2 days, Allan was moved to a
regular room and an oncologist was called in for consultation.
Allan was released from the hospital on August 12 and spent the next 2
½ weeks trying to gain his strength back. On August 24, we received
the final pathology report confirming mesothelioma.
The Search for Treatment Options Begins
That night I was back on the Internet looking for the best hospitals in
the country to treat lung diseases. For hours I went through different
web sites looking for any hope even though I had read enough to know the
outcome of this disease.
 Karmanos Cancer Center,
Karmanos Cancer Center,
Detroit, MI
9/8/99
My guardian angel must have been watching this unending search, because
somehow I ended up at a site indicating areas of asbestos exposure in
Indiana. I sent them an e-mail requesting asbestos information about the
steel mills in northern Indiana. In addition, I informed them of my husband's
diagnosis received that day and asked if they knew of a physician in the
Chicago area or Northern Indiana who specialized in this type of cancer.
I asked them to call me, thinking that like everything else it would take
days, maybe weeks. I forwarded this e-mail at 11:00 PM on a Tuesday night.
At 8:00 AM, Wednesday morning, my phone rang. "Mrs. Ostling, I received
your e-mail. How can I help you? You don't have to go through this
alone. There are things that can be done and we will help you in any way
we can."
This was my introduction to Roger G. Worthington, P.C., soon to be our
lifeline for the future. My new, best friends were to be Roger Worthington,
Trey Smith and Mike Bittner.
That was the first time anyone or anything had given me any hope. They
told me of other similar cases, many with positive outcomes. They told
me about the research being done throughout the country with mesothelioma.
They told me about a foundation that they were helping to create: MARF
(Mesothelioma Applied Research Foundation). The best specialists in the
country were on the board of MARF. That day, I received numerous e-mails
from all three of my newest 'angels', along with several more
phone calls. The very next day, I received an enormous Fed-X package with
volumes of information about mesothelioma, case studies, trials going
on throughout the United States, lists of doctors along with addresses,
phone numbers and e-mail addresses. There was so much to read and digest.
I was astounded to actually find out many people with this disease had
gone through surgery, some removing just the pleura, some the entire lung.
There were studies of people extending their lives by years past the first
doom and gloom dates they were given.
The Local Standard of Care Offers Conventional Cancer Treatment Only
 Brigaham & Women's
Brigaham & Women's
Boston, MA
9/12/99
We saw our oncologist, Dr. Mary Klein, on August 30. Once again, we asked
about any type of surgery, and received the same answer, surgery was not
indicated. We were told the standard of care in our community was chemo
and radiation only. We pressed further telling her about surgeries elsewhere
in the country. Dr. Klein is a very kind, warm-hearted physician. She
understood our search for answers and explained if we lived closer to
university hospitals or research hospitals, perhaps things would be different.
But, again, in our locality, the standard would be chemo and radiation.
Even with that, we were given 7-9 months.
We told Dr. Klein that we had to extend our search for alternative solutions.
She encouraged us to do so, but explained we had to "do something"
or start some type of treatment within 30 days.
Back home, a little stunned by the absence of options and a fairly bleak
future, I picked up the phone and called my angels and said, "We
need your help."
Before I could even figure out where we should go, Roger had e-mailed 3
of the top mesothelioma specialists in the country to introduce us and
plead Allan's case.
Dr. Harvey Pass Responds to Plea for Help
One day later, Dr. Harvey Pass from the Karmanos Cancer Institute in Detroit
was on the phone personally and had also e-mailed us. He agreed to see
us the following week and asked that we get several additional tests prior
to our visit.
The next contact was from Brigham and Women's Hospital in Boston. Dr.
Scott Swanson agreed to see us on September 13 and also requested a few
more tests. From September 3 to September 8, Allan spent his waking hours
at the hospital getting outpatient tests and returning for results. Everyone
was very accommodating in helping us get all the tests and results in
time for our trip east. In the meantime, I had managed to get an appointment
on September 14 with Dr. Roman Perez-Soler, a specialist at the Kaplan
Cancer Institute in New York and another appointment on September 15 with
Dr. Valerie Rusch at the Memorial Sloan Kettering Cancer Center in New York.
First Stop: Dr. Pass in Detroit
 Kaplan Comprehensive Cancer Center
Kaplan Comprehensive Cancer Center
New York, NY
9/14/99
Our whirlwind trip began on September 9, by seeing Dr. Pass in Detroit.
The approach used at Karmanos is very logical and complete. Dr. Pass allowed
us to tape record our entire conversation with him, at least 1 ½
hours. He took Allan's history, did an examination and thoroughly
explained all procedures that might be considered. We left for lunch while
Dr. Pass and the committee of surgeons, pathologists and radiologists
met at noon to discuss each case, look at x-rays, scans, pathology slides, etc.
At 1:15 we met with Dr. Pass again and he explained the committee's
decision. Based on what could be determined from all the records we brought,
the decision was made to attempt a Pleurectomy only (removal of only the
lining of the involved lung). He further stated, he would take a "good
look around" during surgery to determine any further involvement.
If he found anything else, then the procedure would proceed to an EPP
(extra pleural Pneumonectomy - removal of the entire lung). He explained
everything in detail, and then answered an entire page of questions we
had written during lunch. Another 1 ½ hours passed.
I cannot say enough about the thoroughness of Dr. Pass. He tells you "like
it is". He is very frank, but all the time shows tremendous compassion
and respect for the patient. He was very confident, was certainly an expert
in mesothelioma and seemed to be totally committed to his patients. He
knew we were going on to Boston and New York for other opinions. He helped
to explain his colleague's procedures so we would be better prepared
when we got there. He knew we were in a tough spot and was ready to help
in any way he could.
Second Stop: Dr. Swanson at Brigham and Women's Hospital in Boston
We went on to Boston to Dr. Swanson, who explained the procedure being
used at Brigham. Again we tape-recorded the entire consultation. Dr. Swanson
was very accommodating, calm and in personality, very much like Allan.
Allan commented that Dr. Swanson's approach was much like that of
a methodical engineer. He liked his treatment plan and I could see he
was leaning toward Boston.
Third Stop: Dr. Perez-Solar and Dr. Rusch in New York City
The following day we went into New York to see Dr. Roman Perez-Solar. We
did not fit into the protocol he was using at this time, due to the fact
Allan had already had exploratory surgery.
On Wednesday, we went to Sloan Kettering to see Dr. Valerie Rusch. Dr.
Rusch explained her current protocol and also indicated we should seek
an additional biopsy prior to her taking on Allan's case. Dr. Pass
and Dr. Swanson had also brought this up. We had already scheduled the
biopsy in Detroit the following week since that was closest to our home.
The Consensus: Sugery A Must
All the physicians we met indicated the treatment indicated in Allan's
case was some type of surgery. Dr. Pass planned to begin with the minimal
approach pending his findings during surgery and proceed from there if
necessary to remove the lung. Dr. Swanson and Dr. Rusch took an opposite
approach and removed all at the onset.
After our 10-day marathon, we returned home confused and undecided. I spent
the next day typing up hours of tape-recorded notes from Dr. Pass (17
pages) and Dr. Swanson (10 pages). This turned out to be tremendously
helpful when trying to remember answers to questions directed to each
physician.
In my own mind, I had privately decided that Dr. Pass should do Allan's
surgery. However, I did not want to influence his decision in the slightest.
I had made up my mind that whoever he chose, I would support his decision
even if I didn't agree with it.
Decision Time: Which Doctor Is Best for Allan?
While driving home from our second trip to Detroit, we knew we had to make
a decision. Time was running out. I remember asking Allan how would he
approach a decision like this if he were still working at Inland Steel
and had a piece of equipment that was broken down. I asked him if he would
arbitrarily scrap the entire piece of equipment, or would he methodically
seek what was wrong and then repair or replace just the needed parts,
given the rest of the equipment was in good working order and would last
a longer period of time. He stated he would repair or replace just the
needed parts as necessary.
He then looked at me and said, "That just made my decision."
He said, "I wasn't looking at things that way, but for me, it's
the right approach for me too." When we got home, we called Dr. Pass
and asked him to do Allan's surgery.
Dr. Pass Operates for 7.5 Hours
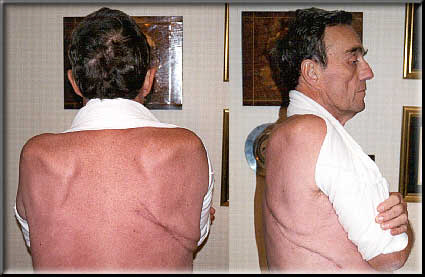 Post Extra-Pleural Pneumonectomy - 11/17/99
Post Extra-Pleural Pneumonectomy - 11/17/99
For us, it was the absolute right decision. The day of surgery Dr. Pass
called me in the surgery waiting room to advise me Allan was ready and
surgery was starting. He had someone call me every 1 ½ hours to
keep me advised of what was happening. Things were looking very positive
when he indicated he was removing just the pleura. Two phone calls later,
they had found further involvement and were removing the entire lung.
I was called upon completion of the surgery (7.5 hours). Later, Dr. Pass
came up and spoke to myself and other family members answering everyone's
questions. Again, I tape-recorded his conversation.
During the next 8 days, Dr. Pass and his residents were the most helpful
and caring people we could ask for. None of that attention stopped when
we left Detroit. The following week when Allan wasn't feeling good,
it took one phone call to Dr. Pass and the next thing I knew, he had arranged
for Allan to get blood transfusions here at our local hospital. He had
to be out of town that evening, and Dr. Pass called us from Texas just
to see how Allan was doing with the transfusions. He arranged for us to
obtain pain control measures when returning to Detroit for check-ups.
Post Operative Chemotherapy Arranged Locally
The decision was made to have Allan's chemotherapy treatments done
here in Indiana. It was becoming too much to make the 4 hour trip to Detroit.
And since we found out his lymph nodes were positive, there will not be
any radiation. Even now, after transferring Allan's care back to Dr.
Klein in Indiana, Dr. Pass wants us to keep in touch. His commitment to
his patients is unequaled.
Jackie Ostling
*** POSTED NOVEMBER 24, 1999 ***